SCHISTOSOMIASIS CONTROL INITIATIVE
The Schistosomiasis Control Initiative (SCI) is a systematized capacity building approach established on rigorous data that seeks to achieve schistosomiasis control and elimination in high-endemic, low-income countries.
CONTINENT
Africa
Country
Ethiopia
Continent
Africa
Country
Burundi, Cote D’Ivoire, Democratic Republic of Congo, Ethiopia, Liberia, Madagascar, Malawi, Mauritania, Mozambique, Niger, Rwanda, Senegal, Sudan, Tanzania, Uganda, Yemen, Zambia, Zanzibar. Case focus on Ethiopia.
Founding year
2003 (work in Ethiopia started in 2013)
Organizational structure
Academic institution
Health focus
Neglected Tropical Diseases, Schistosomiasis
Areas of interest
Health research, Disease control and elimination
Health system focus
Service delivery, Leadership / governance
CHALLENGES
Schistosomiasis affects an estimated 252 million people globally, and 90% of this burden is found in sub-Saharan Africa. It is responsible for 300 000 deaths annually and 70 million disability adjusted live years (Hotez & Kamath 2009; Steinmann et al. 2006; Adenowo et al. 2015). Chronic infection causes caloric malnutrition, growth stunting, anaemia and ultimately organ damage, as well as impairing the response to childhood vaccines (Labeaud, 2009), suppressing the malaria antibody response (Semenya et al., 2012), and increasing the risk of mother-to-child HIV transmission (Secor, 2006).

“SCI’s role and ambition is to see anybody who is infected with schistosomiasis or at risk of schistosomiasis receiving a free drug, praziquantel, which will cure them.”
– Prof Alan Fenwick, Director, SCI

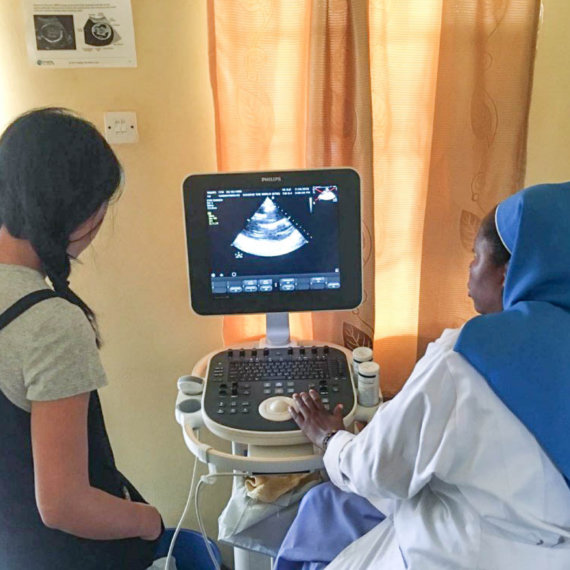
INTERVENTION
SCI’s approach focuses on creating sustainable national programmes through strengthening country capacity. SCI’s intervention begins with a national mapping exercise, which identifies at-risk populations in need of treatment. This is followed by mass drug administration campaigns, which are supported by teachers and community members who receive specific training. SCI leverages drug donations from private companies and coordinates donor funding to maximize impact and efficiency. In the initial stages, countries receive intensive support from SCI to help develop the training programmes; treatment strategies and budgets; governance, reporting, monitoring and evaluation structures; drug procurement and distribution channels; and community mobilisation efforts. After a country is able to execute and implement the programme independently, SCI reduces its support and starts engaging a new country. When SCI withdraws from a country, it ensures that there is sufficient funding and support for the programme to continue.
“We really want and feel very happy if the ministries of health and education embrace this as their programme. Yes, we facilitate it. We give them the money that’s needed to deliver the drugs down the last mile to the schools in the remote areas. We provide them with technical assistance, educational material and the other materials that they need in order to deliver the drugs, but it’s their programme.”
– Prof Alan Fenwick, Director, SCI
Since 2003, SCI reports having been effective in distributing 150 million doses of praziquantel to approximately 40 million people across 18 countries. In 2015, they successfully delivered 25 million treatments, and plan to double that number annually until 2020. All of the SCI partner countries have achieved reductions in schistosomiasis prevalence. In Ethiopia, 85% of affected people were reached through the April and November 2015 campaigns.

CASE INSIGHTS
The SCI case study shows that developing countries can be successful in eliminating neglected tropical diseases if they receive comprehensive support and ongoing mentorship to strengthen their local research, technical and delivery capacity. It also illustrates how partnerships and collaboration with the private sector provide an opportunity to unlock scarce resources, especially essential medicines, which could support the public sector in fulfilling its delivery mandate. The case demonstrates how pooled and co-ordinated donor funding is an effective mechanism for national programmes to achieve their intended impact. A single aligned financial reporting structure increases the efficiency of spending allocation and reporting.
“When SCI was first set up in 2003, for the first four or five years it was really proving the concept that schistosomiasis and STH could be treated at national scale with countries owning the programmes. I think that’s been really innovative.”
– Dr Michael French, SCI Ethiopia Programme Manager