Imaging the World, Africa
A district-led programme that operationalizes the national community health worker strategy to promote quality maternal, new-born, and child health.
CONTINENT
Africa
COUNTRY
Uganda
Location
Uganda
Health Focus
Maternal and Child Health, community
Website
www.imagingtheworld.org
Founding year
2008
Organizational structure
Social Enterprise
Actors involved
Non-State, Other Sectors and State actors
Programme Focus
Service Delivery, Technology
Health System Focus
Human Resources for Health, Products
CHALLENGE
Two thirds of the world’s population lack access to efficient diagnostic imaging. At least one ultrasound scan before 24 weeks of gestation for a pregnant woman is recommended for gestational age estimation, to improve detection of foetal anomalies and multiple pregnancies, and to improve a woman’s pregnancy experience (WHO 2016).
However, due to the inadequacy of human resources for health in low-income countries (radiologists, sonographers, technologists) and the infrastructure required for imaging systems, most rural pregnant mothers cannot access ultra sound services. Patients often need to travel long distances to access these services at district hospitals or urban centres, where imaging centres are often located.
Imaging the world thus ensures that rural pregnant women can access low cost obstetric ultra sound imaging at lower level health facilities, for birth planning and to rule out pregnancy complications.

“In Nawanyago Health Centre, 23% of mothers who have attended antenatal and had the scan have chosen to deliver from Kamuli Mission Hospital. Depending on the mothers’ conditions like how the placenta is lying, the mother is better prepared for normal delivery or C- section”
– Dr Matovu Alphonse, Program officer, ITWA
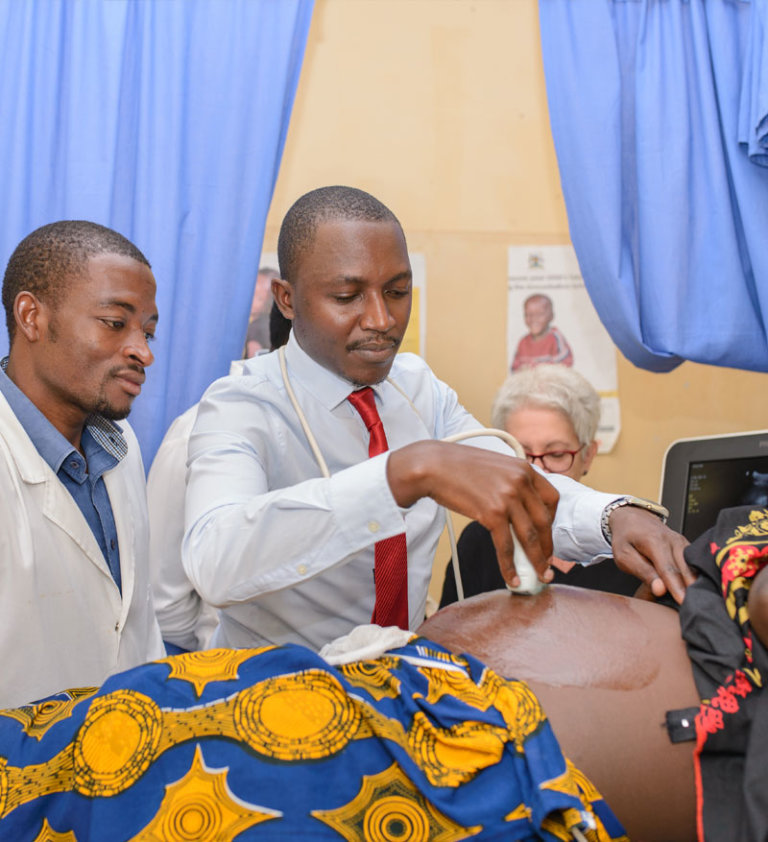
INTERVENTION
The programme involves training identified nurses and midwives in selected lower level health facilities (HC III) to make ultrasound sweeps between specific land marks of the abdomen, to capture multiple clips that are compressed to a size of a still photo and uploaded over cell phone network to a secure system.
An accredited external reviewer (who may be in the country or abroad) receives the images for interpretation and a short report of the findings is sent via Short Message Service to the nurse/midwife’s cell phone.
The ultra sound cost is much lower than what is charged in the private health facilities. The pregnant women contribute 5,000 Shs, which is approximately five times lower than what would be paid in a private health facility. This is used to pay for consumables necessary for the ultrasound process like gel, electricity, and internet costs. The health facility staff are trained for 2 months, examined and supervised by expert radiologists.
“Most of the obstetric findings are normal but we sometimes find abnormalities such as the baby lying in a different position and other abnormalities. It has helped me determine which mothers can be retained here or give early referral to other facilities.”
– Carol Kwikiriza, Clinical Officer, Nyakatare HC III, Kanungu District
Over 200,000 scans have been performed over a period of 6 years, increasing antenatal visits by 70% in health centres employing the Imaging the World model. Twenty-three (23%) of the scans have identified pregnancy complications, which have resulted in specialized care that pregnant women might otherwise not have received.


CASE INSIGHTS
“Given all the advantages like early detection of complications and risks in pregnancy detected, it has helped mothers get referred on time and also attracted mothers to attend antenatal care.”
– Sande Moses, Clinical Officer, Nyamwegabira HC III, Kanungu District
